Spinal balance anteriorization is associated with cognitive decline
- Share
- Tweet
- Send to email
A research report on screening for cognitive decline in citizens’ motor examinations by Hikaru Nishimura, an occupational therapist in the Rehabilitation Center of Shinshu University Hospital, was published in the international science journal, Scientific Reports.
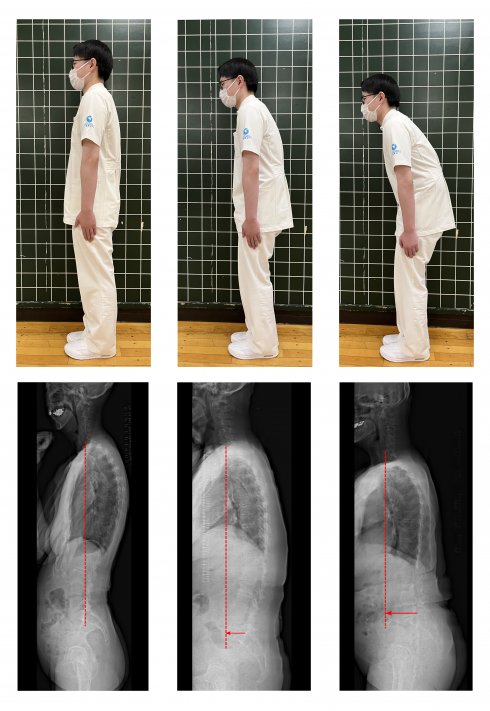
The posture of the spinal column assessed by the examination. The left shows a balanced front-back posture of the spinal column, while the center and the right are in the upper body forward to the pelvis, and the center of gravity ahead. The center of gravity tends to move forward in the elderly. By evaluating this, it is possible to detect a mild decline in cognitive function.
Since 2014, the Department of Orthopaedic Surgery of Shinshu University School of Medicine, and the Rehabilitation Center of Shinshu University Hospital have collaborated with the town of Obuse and New Life Hospital to conduct "the Obuse study", an epidemiological study based on the motor function examinations of the citizens. Occupational therapist Hikaru Nishimura, a member of the spine research group of the Obuse Study, together with Senior Assistant Professor Shota Ikegami of the Department of Rehabilitation Medicine, Professor Jun Takahashi of the Department of Orthopaedic Surgery, and others, conducted a screening of cognitive function decline by assessing spinal sagittal balance based on a radiological approach in the examinations of the citizens aged 50 to 89 years old. The result was reported in the international journal Scientific Reports (Impact factor 4.379).
Mild cognitive impairment is a stage between healthy and dementia and is estimated to occur in 10-20% of the elderly. Because this condition can be reversible to its original state, identifying whether a person has mild cognitive impairment is important for preventing future dementia. The spine research group of the Obuse Study has shown in previous studies that motor function decline occurs along with cognitive decline in the elderly and that motor function decline is manifested as changes in posture, leading to the hypothesis that it may be possible to screen for cognitive decline by detecting postural changes specific to the elderly and found that this hypothesis was correct.
Sagittal vertical axis (SVA) is a typical indicator of spinal sagittal balance, and SVA is the length of a horizontal line from the posterior superior border of the sacral vertebral body to the anterior center of gravity of the seventh cervical vertebra in a plain lateral radiograph. In a balanced posture, the C7 vertebral body is located directly above the sacrum, so the SVA is around 0 cm. However, as the back rounds with getting older, the head gradually moves forward and the SVA increases to 5 cm, 10 cm, and so on. Nishimura et al. asserted that in male cases over 50 years old and who has an SVA of 10 cm or more, over 70 years old and has an SVA of 9 cm or more, or over 80 years old and has an SVA of 7 cm or more, there is a high possibility that cognitive decline is occurring. In addition, they stated that in women cases over 50 years of age, regardless of age, if the SVA is 7 cm or more, there is a high possibility that cognitive decline is also occurring.
Cognitive decline in the elderly is considered to be an element of "frailty", a condition unique to the elderly in which they tend to lose their health and require nursing care, in combination with the decline in physical function and loss of social roles that occur at the same time. Based on the results of this study, the spine research group of the Obuse Study hopes to use the results of this research to help prevent future required nursing care by identifying frailty at an early stage through postural examinations of citizens and providing appropriate intervention.
Title of the report and Authors:
Authors: Nishimura H, Ikegami S, Uehara M, Takahashi J, Tokida R, Kato H.
Title: Detection of cognitive decline by spinal posture assessment in health exams of the general older population. (Sci Rep. 2022 May 19;12(1):8460.)
For details, please refer to the URL below.
https://www.nature.com/articles/s41598-022-12605-7.pdf
EurekAlert!
https://www.eurekalert.org/news-releases/955581